The case for HIV screening
22 June, 2004
Summary| • | Since 1997, heterosexual intercourse has become the largest and fastest growing exposure category for human immunodeficiency virus (HIV) diagnoses made in the UK; |
| • | A large majority of heterosexual HIV infections recently diagnosed in the UK were acquired in Africa; |
| • | The cost of managing an HIV-positive patient in the UK is around £15,000 per year; |
| • | The total potential cost to the NHS of treating cases of African origin diagnosed in the UK over the last five years is over £1 billion; |
| • | The test for HIV is highly accurate; |
| • | It would be feasible to require HIV screening for those who are not refugees, who are immigrating for a substantial period and who are not entitled to free movement under European law; |
| • | This would reduce the national burden of disease, ensuing treatment costs and future transmission within the United Kingdom; |
Introduction - some facts
1. The spread of HIV and other sexually transmitted infections in the UK is now increasingly influenced by patterns of migration and overseas travel.[1] Specifically in relation to HIV, the Health Protection Agency has concluded the following:
| • | Around three-quarters of the 3,152 heterosexually acquired HIV infections newly diagnosed in the UK in 2002 were probably acquired in Africa [2] |
| • | Of HIV-infected heterosexuals seen for care in 2002, 66% were black-African, a 330% increase (to 8,262) since 1997; [3] |
| • | By contrast, diagnoses of HIV infection acquired heterosexually within the UK amounted to only 275 reported for 2002; an increase of 128 compared to 1998. The majority of these individuals were probably infected through partners who acquired their infections outside Europe; [4] |
| • | For the first time [in 2003] there was an indication that the prevalence of previously undiagnosed HIV infection may have risen amongst heterosexual clinic attendees who were born in the UK. [5] |
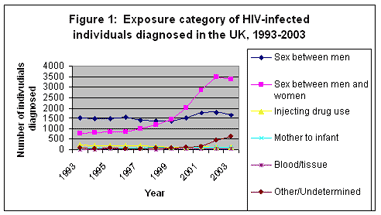
2. Figure 1 [6] shows that the rate of HIV diagnosis among heterosexuals in the UK has taken off, surpassing the rate of diagnosis among homo/bisexuals in 1999 and continuing to rise more strongly than any other exposure category in every subsequent year.
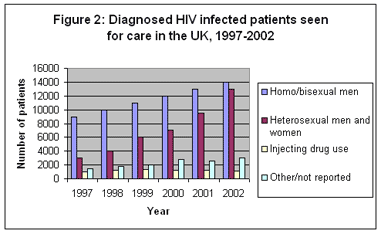
3. Figure 2 [7] shows that the patterns for treatment of HIV in the UK broadly reflect the changing trends in the patterns for diagnosis, with most growth in the heterosexual exposure category.
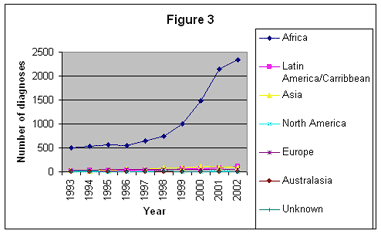
4. Figure 3 above shows, by region of the world, the number of HIV infections newly diagnosed in the UK, presumed to have been acquired heterosexually from partners abroad, from 1993-2002. The dominance of Africa in new diagnoses, already very marked in 1993, took off in 1997 and has been extended considerably in every subsequent year. Since 1999, infections acquired in South Eastern Africa, and in particular Zimbabwe, have dominated [8].
The Cost of Treatment to the NHS
5. According to the National Association of NHS Providers of AIDS care and Treatment (PACT), the cost of managing a patient with HIV is £15,000 per year. The total cost of treatment and care in 2002-03 will be £345 million [9] . It is estimated that the average lifetime treatment cost for an HIV-positive person is between £135,000 and £181,000 [10] . From 1998-2002 there were 7,706 diagnoses in the UK of HIV thought to have been heterosexually acquired in Africa. On the Department of Health’s cost estimates, the cost of treating just this one group will be between £1.04 billion and £1.39 billion
The effectiveness of screening
6. Screening immigrants for tuberculosis, another globally-recognised public health risk, is an internationally widespread policy. The tools used for screening for this disease, however, are highly imperfect. Research [11] suggests that the sensitivity (proportion of true cases detected) of X-ray screening for TB is around 75% and that specificity (the proportion of true negative cases detected) is about 99%. Applying these proportions to the prevalence rate of TB in Zimbabwe, of 600/100,000, Richard Coker calculates that if 10,000 immigrants from Zimbabwe were screened, 69% of those found by the screening process to have the disease would not in fact have it (the “false positives”). These levels of accuracy are clearly too low to justify TB screening as a public policy basis for discriminating between prospective immigrants.
7. Antibody tests for HIV, however, are highly specific and sensitive; with confirmatory tests, rates for both are close to 100% [12] . Furthermore, the 3-month “window period” between infection and the reliable development of antibodies has been less problematic since the development of tests which can reliably detect early infection [13].
8. In a recent report [14], the All-Party Parliamentary Group on AIDS came down heavily against the idea of screening migrants for HIV upon entry to the UK. Arguments for this conclusion included the following:
| • | UNHCR and UNAIDS guidance of 1998 stated that “There is no public health rationale for restricting liberty of movement or choice of residence on the grounds of HIV status” [15]; |
| • | Restrictions of movement based on HIV status are resource-intensive [16]; |
| • | Testing migrants for HIV upon entry into the UK sends out a false sense of security to the general public that they are not at risk of acquiring HIV and that only immigrants and asylum seekers carry this risk [17]; |
| • | Singling out HIV as an illness which we would like to keep out of the UK risks discouraging individuals who are already in the UK from testing [18]; |
| • | Ensuring a welcoming environment for pre and post-test counseling in the context of mandatory testing upon entry would be a serious challenge and could risk infringing upon the rights of individuals [19]; |
| • | Mandatory testing would risk HIV becoming further stigmatised [20]. |
9. Since asylum seekers arrive unannounced, they cannot be tested in advance. Neither can they be legally denied the right to seek asylum by reason of a positive HIV test result.
10. Screening pre-arrival raises different questions. Those immigrating for economic (or educational) purposes but who do not enjoy free movement rights under European law could be denied entry by reason of a positive HIV test result.
11. Whilst it would not be practicable to screen all visitors, effective criteria could be put in place so that screening was required for people wanting to immigrate for substantial periods, such as students and work permit holders. In 2002 about 20,000 students and 10,000 Work Permit holders came from sub-Saharan Africa. Currently 46 countries require HIV tests before immigration [21]. Australia, for example, has a network of approved medical examiners who conduct any necessary tests at the applicant’s expense.
12. Refusing entry to immigrants infected with HIV would reduce the national burden of disease, ensuing treatment costs and future transmission within the United Kingdom. It would not, of course, tackle the problem of the global HIV epidemic, but that is a separate (albeit important) matter.
13. Compulsory screening for diseases other than HIV may be appropriate for people falling into certain other categories: for example, under the Australian Regulations, pregnant women, children for adoption and unaccompanied minors must be screened for hepatitis.
Conclusion
14. There is clear evidence that the pool of HIV infection in the UK is growing and that the infection and treatment rate among heterosexuals in the UK has taken off. There is also clear evidence that Africa has been by far the most significant overseas source of HIV infection for diagnoses made in the UK over the last decade, and its lead over other regions of the world in this regard continues to grow [22]. The potential cost to the NHS of cases of African origin diagnosed over the last five years for which figures are available is in excess of £1 billion. At present, there is no mandatory screening for communicable diseases for immigrants to the UK as there is for many other countries, yet there is scope to introduce highly accurate HIV screening for those immigrating for economic or educational purposes, for substantial periods, who are not entitled to free movement rights under European law. The implementation of such screening would be beneficial to public health and to public funds in the UK and to actual and potential immigrants themselves. The objections are minor in comparison.
ANNEX A
Asylum applicants
An applicant’s health should be, and indeed is, regarded as irrelevant to the consideration of their case under the 1951 Refugee Convention. However, some who suffer from AIDS have sought to use Article 3 of the European Convention on Human Rights, which provides that “no one shall be subjected to torture or to inhuman or degrading treatment or punishment”. In a test case in the Court of Appeal on 16 October 2003, the Court found that; “the fact that the applicant’s life expectancy will be reduced, even substantially reduced, because the facilities in the receiving country do not match those in the expelling country is not sufficient to engage Article 3. Something more is required” [23]. The appeal was dismissed, thus permitting the removal of failed asylum seekers even if they suffer from HIV/AIDS, unless there is “some special feature that gives rise to particularly compelling humanitarian considerations” [24].
ANNEX B
Visitors
The following categories of patient are exempt from charges for treatment the need for which arose during their visit to the UK:
| • | nationals, or refugees, or stateless persons and their family members resident in European Economic Area (EEA) member states and Switzerland; plus, non-EEA nationals who are legally resident and insured in an EU member state (except Denmark); |
| • | UK state pensioners who have either lived lawfully in the UK for 10 continuous years or have been employed by the UK government for 10 continuous years at some point, or their spouse or school-age children; |
| • | people from non-EEA countries with which the UK holds bilateral (or reciprocal) health care agreements; |
| • | people who are without sufficient resources to pay the charge and who are nationals of a country which is a contracting party to the European Convention on Social and Medical Assistance 1954; |
| • | people who have lived lawfully for 10 continuous years in the UK but who are now living in an EEA member state or Switzerland, or a non-EEA country (other than Israel) with which the UK has a bilateral (or reciprocal) health care agreement, and their spouse and school-age children; |
| • | an authorised companion (who need not be a spouse) of an individual who has been designated exempt by the Secretary of State on exceptional humanitarian grounds [25]. |
Footnotes
| [1] | Renewing the Focus, HIV and other Sexually Transmitted Infections in the United Kingdom in 2002, An update: November 2003, Ch 13.2 |
| [2]` | ibid, Ch 3, Table 2 |
| [3] | ibid, Ch 12.3 |
| [4] | ibid, Ch 3.2.1 |
| [5] | ibid, Ch 3.4.2 |
| [6] | Figure 1 uses data from the Health Protection Agency’s AIDS/HIV Quarterly Surveillance Tables No. 62: 04/1, published in May 2004. The apparent fall in the two exposure categories involving sex and the corresponding rise in undetermined diagnoses is due to the lack of detailed information to date on diagnoses made in 2003, as compared with previous years. |
| [7] | The data source for Figures 2 and 3 is HIV/AIDS reports received by the end of June 2003, as cited in Renewing the focus, HIV and other Sexually Transmitted Infections in the United Kingdom in 2002, An update: November2003. For the most recent years, 2001 and 2002, the figures will continue to rise as the Health Protection Agency receives and collates further data. |
| [8] | Renewing the focus, HIV and other Sexually Transmitted Infections in the United Kingdom in 2002, An update: November 2003, Ch 3.2.1 |
| [9] | Sexual Health: Third Report of Session 2002-03, House of Commons Health Committee, May 2003, p46 |
| [10] | The National Strategy for Sexual Health and HIV, Department of Health, 2001, p11 |
| [11] | Toman, 1981, as cited in Coker Migration, public health and compulsory screening for TB and HIV, at p22 |
| [12] | ibid, at p23 |
| [13] | Rawal et al, as cited in Coker at p24 |
| [14] | Migration and HIV: Improving Lives in Britain, July 2003 |
| [15] | ibid, para 53 |
| [16] | ibid, para 53 |
| [17] | ibid, para 55 |
| [18] | ibid, para 57 |
| [19] | ibid, para 59 |
| [20] | ibid, para 62 |
| [21] | Coker at p9 |
| [22] | see Figure 3 above |
| [23] | N v Secretary of State for the Home Department [2003] EWCA Civ 1369, per Lord Justice Dyson at para 47 |
| [24] | ibid at para 49 |
| [25] | Proposals to Exclude Overseas Visitors from Eligibility to Free NHS Primary Medical Services, Department of Health Consultation Document, May 2004, pp20-21 |
